Stem Cell for Knee Replacement: A 2026 Patient's Guide
For individuals navigating chronic knee pain, the conversation has historically led to one primary conclusion: surgery. Today, stem cell therapy is fundamentally reshaping that paradigm. It represents a shift away from managing symptoms or replacing a joint, and toward activating the body’s innate capacity for healing.
Unlike a knee replacement, this regenerative approach utilizes targeted injections to reduce inflammation, alleviate pain, and potentially delay or eliminate the need for major surgery. This guide explains how allogeneic stem cell therapy offers a sophisticated, non-surgical path to preserving your natural knee and reclaiming an exceptional quality of life.
A New Horizon for Knee Health
Chronic knee pain stemming from osteoarthritis or a past injury does more than just cause discomfort. It can profoundly impact your ability to lead an active life, limiting mobility, interrupting sleep, and sidelining you from the activities you love.
For years, the treatment path was linear: begin with pain medication, progress to corticosteroid injections, and ultimately, face a total knee replacement. While surgery is an effective solution for end-stage conditions, it is accompanied by significant downtime, a demanding recovery, and the reality of an artificial joint.
Today, regenerative medicine presents a compelling alternative for many. The goal is no longer to simply mask pain, but to intervene at a biological level. By addressing the underlying inflammation and tissue degradation causing the symptoms, we can help preserve your natural joint structure and function for years to come.
Comparing Treatment Philosophies
The core difference between stem cell therapy and knee replacement lies in their fundamental objectives. One aims to repair and preserve the joint you were born with, while the other is designed to replace it entirely.
| Treatment Approach | Stem Cell Therapy (Allogeneic) | Total Knee Replacement Surgery |
|---|---|---|
| Primary Goal | Preserve the natural knee joint | Replace the damaged joint with an implant |
| Mechanism of Action | Reduces inflammation and supports tissue repair | Removes damaged cartilage and bone |
| Invasiveness | Minimally invasive injection | Major invasive surgical procedure |
| Recovery Time | Minimal downtime, typically days | Extensive rehabilitation over months |
This distinction is crucial, especially for active adults who wish to avoid the long-term implications of major surgery. By focusing on preservation, candidates for stem cell for knee replacement alternatives can pursue a strategy that aligns with a longevity-focused approach to wellness—one that aims to maintain the body's inherent strength and function.
You can learn more about other non-surgical approaches in our detailed guide on alternatives to knee replacement surgery.
Stem cell therapy shifts the focus from joint replacement to joint preservation. For patients with mild-to-moderate osteoarthritis, this approach offers a strategic opportunity to manage pain and improve function without the extensive recovery and risks associated with major surgery.
This guide provides a clear, evidence-based overview of how this advanced therapy works, who it is best suited for, and what you can expect from the treatment process, empowering you to make an informed decision about your knee health.
How Stem Cell Therapy Works for Knee Conditions
To understand how stem cell therapy offers such a compelling alternative to knee replacement, it is essential to look beyond the concept of "regrowing" a joint. The biological process is far more sophisticated. It is about orchestrating the body’s own powerful repair systems directly within the knee.
At Longevity Medical Institute, we utilize allogeneic mesenchymal stem cells (MSCs). These are exceptionally potent, youthful cells sourced from the umbilical cords or placenta of meticulously screened, healthy donors. By using these pristine cells, we ensure we are working with a vibrant and highly concentrated force for healing, which is critical for achieving a powerful therapeutic response.
Think of these MSCs less as simple building blocks and more as intelligent biological directors. When introduced into the knee, they do not merely transform into new cartilage. Instead, they release a cascade of powerful signaling molecules—such as growth factors and cytokines—that modulate the joint's environment and direct the healing process.
Calming Inflammation and Supporting Repair
Chronic inflammation is the primary driver of pain and cartilage degradation in an osteoarthritic knee. Allogeneic MSCs are exceptionally effective at bringing this inflammation under control.
They function as a sophisticated command system, calming the overactive immune cells that attack the joint lining and cartilage. This reduction in inflammation is often the first benefit our patients notice, leading to significant pain relief and diminished stiffness.
Once the inflammatory cascade is suppressed, the body has an opportunity to heal. The growth factors released by the MSCs then encourage existing cells within the knee to function more effectively, which helps protect remaining cartilage and can slow further degradation.
One can think of it as bringing in an expert management team to revitalize a struggling factory. The managers (the MSCs) do not replace all the workers; they organize them, provide better instructions (signaling molecules), and create an environment where the entire system can operate more efficiently and productively.
The Importance of Quality and Clinical Standards
The success of any stem cell therapy is directly linked to the quality, purity, and viability of the cells used. This is where clinical rigor is non-negotiable and what distinguishes a legitimate medical procedure from an unproven one. Our on-site, COFEPRIS-licensed laboratory operates under the strictest protocols to ensure every dose of MSCs meets the highest international standards for both safety and potency.
This commitment to quality is crucial, especially as the field expands. The global market for knee stem cell therapy is experiencing incredible growth and is projected to reach $438.74 million by 2025, with a compound annual growth rate of 18.7%. This expansion is driven by the rising number of individuals affected by knee disorders worldwide. You can explore more on these market growth trends and statistics.
By choosing a facility with verifiable credentials and transparent laboratory processes, you ensure the therapy you receive is based on sound science. Understanding this science is the first step, and our guide on stem cell injections for knee pain provides more detail on what to expect. This focus on quality and precision is how we harness the full potential of regenerative medicine for knee conditions.
Stem Cell Therapy vs. Knee Replacement: A Detailed Comparison
When confronting chronic knee pain, the path forward often narrows to two distinct philosophies. One involves surgically replacing the joint, while the other focuses on preserving and repairing it from within. It is a significant choice, and understanding the fundamental differences between stem cell therapy and a total knee replacement is the first step toward making a confident decision.
This is not a simple list of pros and cons. Instead, we will examine the critical factors that matter most to patients: the physical impact of the procedure, the expected recovery timeline, and the potential for long-term joint health.
Invasiveness and Recovery: A Tale of Two Timelines
The most immediate and stark difference between these two treatments lies in their impact on your body and the time required to return to full activity.
A total knee replacement is a major, invasive surgery. It is an effective solution that involves removing damaged cartilage and bone and replacing those surfaces with metal and plastic implants. This requires a hospital stay, a significant period of pain management, and an extensive rehabilitation process that can easily last 3 to 6 months—or longer—before full function is restored.
In contrast, allogeneic stem cell therapy is a minimally invasive procedure performed in our clinical setting. Using high-resolution ultrasound for guidance, we perform a precise injection directly into the knee joint. There are no incisions, no general anesthesia, and no hospital stay. Patients walk out of the clinic shortly after the procedure and can typically return to light, normal activities within a day or two.
This vast difference in recovery is a defining factor, especially for active individuals or professionals who cannot afford to put their lives on hold for months.
Outcomes and Long-Term Preservation
Another key consideration is how each approach aligns with your long-term health goals. A knee replacement is often the definitive solution for end-stage, bone-on-bone arthritis. By removing the source of pain, it can provide tremendous relief. However, an artificial joint is a mechanical device with a limited lifespan, and revision surgeries may eventually be necessary.
Stem cell therapy operates from a different philosophy: preservation. The objective is to fundamentally change the environment inside your knee. By controlling harmful inflammation and providing powerful signals that support the body’s own repair mechanisms, we aim to protect existing cartilage, slow the progression of osteoarthritis, and improve the overall health of the joint. It is about preserving the natural knee you were born with, potentially delaying or even avoiding the need for surgery.
After a knee injury, the body can follow two paths—one toward healing, and the other toward chronic impairment and degeneration. This is where a targeted intervention can make all the difference.
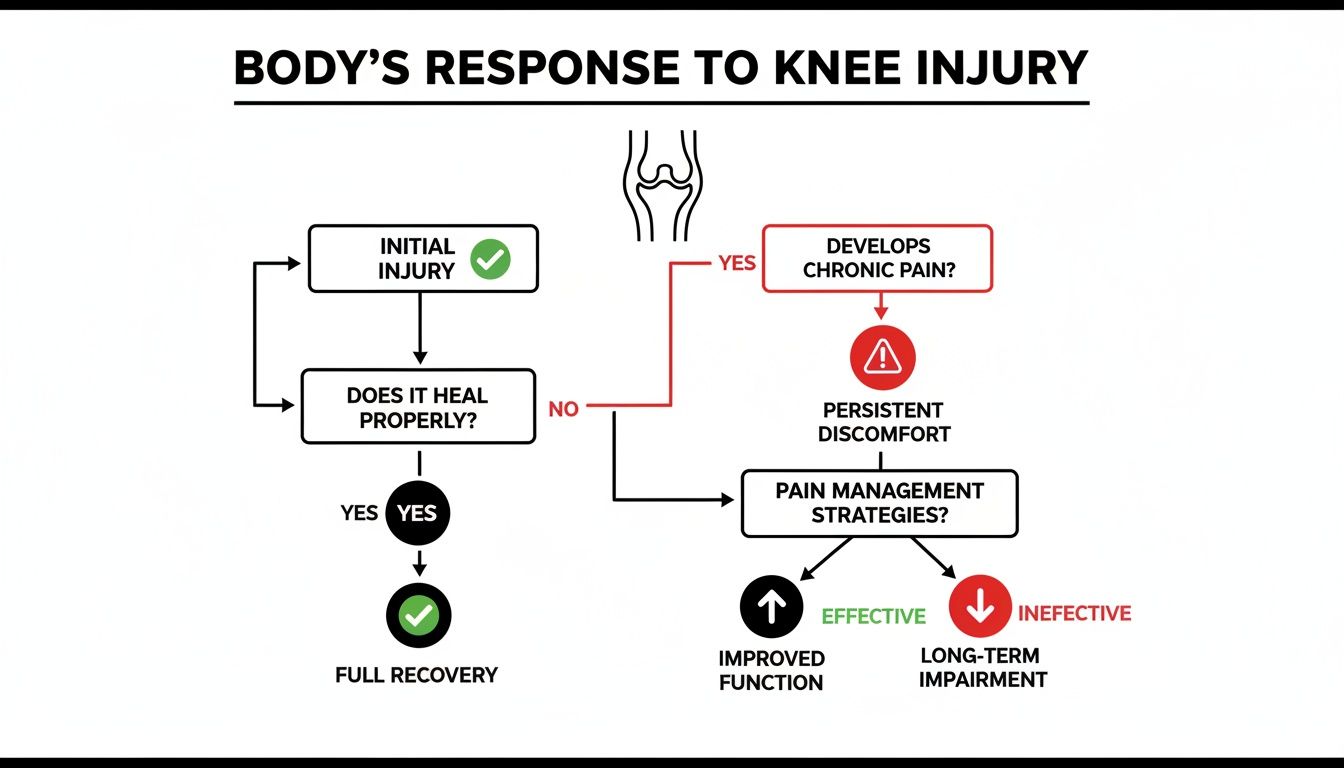
As illustrated, the objective is to guide the body’s response away from the cycle of chronic pain and toward true healing.
To provide greater context, we have created a side-by-side analysis of the key decision factors our patients consider when evaluating these two options.
Comparative Analysis: Stem Cell Therapy vs. Total Knee Replacement
| Decision Factor | Allogeneic Stem Cell Therapy | Total Knee Replacement Surgery |
|---|---|---|
| Primary Goal | Joint preservation and biological repair | Joint replacement and pain elimination |
| Invasiveness | Minimally invasive (ultrasound-guided injection) | Highly invasive (major open surgery) |
| Procedure Time | Approximately 30-45 minutes | 1-2 hours, plus hospital stay |
| Anesthesia | Local anesthetic only | General or spinal anesthesia |
| Recovery Time | Return to light activity in 1-2 days | 3-6 months of intensive rehabilitation |
| Pain Level | Mild, temporary soreness at injection site | Significant post-operative pain |
| Ideal Candidate | Mild-to-moderate osteoarthritis; active individuals | Severe, end-stage "bone-on-bone" arthritis |
| Longevity | Aims to extend the life of the natural joint | Implant has a limited lifespan (10-20% may need revision) |
| Risks | Minimal (low risk of infection or reaction) | Infection, blood clots, implant failure, nerve damage |
This table clarifies that these are not interchangeable treatments; they are designed for different stages of joint disease and for patients with distinct priorities and goals.
A Scenario-Based Comparison
To bring these differences to life, let’s consider a common patient profile: a 55-year-old who loves to hike but is being held back by moderate knee osteoarthritis.
Path 1: Knee Replacement: Following surgery, they would face a minimum of 3 to 6 months of intensive physical therapy. Hiking would be precluded for an extended period. While they would likely return to the trails, new restrictions on high-impact activities may be necessary to protect the implant for the long term.
Path 2: Stem Cell Therapy: After the injection, they would rest for a short period and then quickly return to low-impact exercise. They could be back on gentle hiking trails within a month or two, experiencing progressive improvements in pain and function as the therapy works to heal the joint from within.
The choice truly hinges on the stage of the disease and the patient's goals for their future. For severe, end-stage arthritis, surgery remains the gold standard. For mild-to-moderate cases, stem cell therapy offers a powerful opportunity to manage the condition proactively and preserve an active lifestyle.
This proactive approach is gaining significant traction in the medical community. There are now 224 registered interventional studies worldwide examining stem cell therapies for knee osteoarthritis. The published data is compelling, with studies showing pain reductions of 50-66% at 12 months and functional improvements in 60-85% of patients with mild-to-moderate cases.
By contrast, while nearly 800,000 knee replacements are performed each year in the U.S., it is important to note that for 10-20% of patients, revision surgery becomes necessary within a decade.
Understanding the clinical environment where these procedures are performed is as important as the therapy itself. You can get a sense of what distinguishes a high-quality facility by learning more about our state-of-the-art surgical center.
Comparing the Financial Investment in Your Knee Health
Making a clear-headed decision about your knee health requires looking beyond the initial price of a procedure. It is about understanding the complete financial picture of your long-term mobility. When weighing stem cell therapy against knee replacement, it is crucial to consider everything from the upfront investment to the often-overlooked costs of a lengthy and disruptive recovery.
The financial models for these two paths could not be more different. For patients in the U.S. and Canada, the out-of-pocket expense for a knee replacement can be staggering, even with insurance. The final cost is a complex composite of hospital fees, surgeon and anesthesiologist charges, diagnostic imaging, and—critically—the ongoing expense of post-surgical physical therapy that can continue for months.
A Look at the Numbers
Regenerative medicine, on the other hand, presents a much more direct financial model. While typically not covered by insurance, the upfront investment is predictable and often represents a far greater overall value when all factors are considered.
In 2026, costs for stem cell therapy for knees can range from $3,500 to $25,000 per knee, a spread reflecting the quality of the cells, the clinic’s location, and the comprehensiveness of the protocol. Compare that to a traditional knee replacement, which averages $30,000 to $50,000 for an uninsured patient in the United States.
This stark cost difference is a primary reason Mexico has become a leading destination for medical travel, with over 1.2 million people visiting each year for world-class care at a more accessible price point. It is a comparison that illustrates why so many North Americans are now looking abroad for procedures like stem cell for knee replacement alternatives.
The Hidden Costs of Surgical Recovery
The true financial toll of knee replacement surgery extends far beyond the hospital invoice. The recovery itself introduces a new set of expenses that are easily overlooked during the planning stages.
Lost Income: Being unable to work for months can mean a substantial loss of earnings, a particularly harsh reality for self-employed professionals or anyone without robust short-term disability coverage.
Prolonged Rehabilitation: Co-pays for numerous physical therapy sessions can accumulate quickly, becoming a significant secondary financial drain.
Assistive Devices: The need for walkers, crutches, or modifications to one's home adds another layer to the overall financial burden.
Because stem cell therapy involves minimal downtime, most patients return to work and their daily routines within a few days, effectively eliminating these secondary economic impacts.
The total value of a treatment is not just its price tag. It is the cost of the procedure plus the cost of recovery, measured in both dollars and lost time. A minimally invasive approach preserves not only your joint but also your financial and personal independence.
By choosing a path that avoids a long and difficult rehabilitation, you are making a smart investment in both your immediate and future well-being. We provide a detailed breakdown of what our treatment packages include in our guide to understanding stem cell therapy cost. Our goal is to offer a comprehensive wellness experience that delivers exceptional value by prioritizing your health, time, and long-term mobility.
Determining if You Are an Ideal Candidate for Stem Cell Therapy
Not everyone with knee pain is a suitable candidate for stem cell therapy. This is not a universal solution; it is a precise medical therapy where success is fundamentally tied to careful patient selection. A thorough, honest evaluation is the critical first step to determine if this approach truly aligns with your knee's condition and your personal health goals.
The most important factor we assess is the stage of your osteoarthritis. We have found that regenerative therapies deliver the best, most lasting results for individuals with mild-to-moderate (Grade 1-3) osteoarthritis. In these earlier stages, there is still a meaningful amount of cartilage to preserve, and the joint’s internal environment is far more receptive to the powerful anti-inflammatory and healing signals from the stem cells. Our goal is to intervene before the damage becomes irreversible.
Who Benefits Most from This Approach
Ideal candidates are typically those whose goal is to preserve their natural joint and improve its function, not just manage pain. We consistently see the greatest potential for positive outcomes in these specific groups.
Active Adults with Early to Mid-Stage OA: Individuals who want to maintain an active lifestyle—whether that means playing tennis, hiking, or keeping up with grandchildren—but find themselves limited by growing pain and stiffness.
Patients with Specific Cartilage or Meniscal Injuries: Those who have a localized cartilage defect or a meniscal tear that has not yet led to widespread, end-stage arthritis.
Individuals Seeking to Proactively Delay Surgery: Patients who understand their condition is degenerative and want to take a decisive, biological step to preserve their own joint for as long as possible.
This proactive approach is centered on managing the long-term health of your joint, making it an excellent stem cell for knee replacement alternative for those who are not ready for, or wish to avoid, major surgery.
Understanding the Limitations: Transparency Is Key
While stem cell therapy is a powerful tool, it is not a panacea. For individuals with severe, end-stage (Grade 4) osteoarthritis—often described as "bone-on-bone"—the structural damage to the knee is simply too extensive for this approach to be effective. At this stage, there is little to no cartilage left to preserve or support, and the joint's architecture is significantly compromised.
For patients with Grade 4 osteoarthritis, total knee replacement surgery remains the most effective and definitive solution. Our commitment is to provide an honest, clinically sound recommendation, and we will always guide patients toward the treatment that offers them the best possible outcome.
This transparency is fundamental to our practice. Attempting regenerative therapy on a joint that lacks the foundational structure for it to work would be a disservice to the patient.
A comprehensive diagnostic process is essential to make this determination. We always begin with a detailed medical history and a hands-on physical examination, but we often go deeper with advanced imaging. We may utilize tools like an AI-enhanced MRI to get a precise picture of your cartilage thickness, bone health, and the overall inflammatory state inside the joint. This data-driven approach ensures we place you on the most appropriate and effective treatment path for your specific condition.
The Patient Experience at Longevity Medical Institute
Deciding to move forward with regenerative medicine is a significant step. We believe the entire experience—from your first phone call to your final follow-up—should feel as restorative and well-managed as the therapy itself.
At Longevity Medical Institute, we have designed a physician-led journey that provides clarity, comfort, and confidence at every turn. It is a true partnership built on trust and an unwavering commitment to exceptional clinical care.
Your path to improved knee health starts with a remote consultation. During this session, you'll have a direct conversation with our clinical team to talk about your knee pain, go over your medical history, and outline your objectives. We offer in-house scanning using MRI, ultrasound, or X-ray to evaluate the situation, and we can also review your existing MRIs or X-rays to determine if a stem cell for knee replacement alternative is suitable for you.
Your In-Clinic Evaluation and Treatment
Upon your arrival at our clinic in San José del Cabo, your care shifts to a hands-on, in-person experience. We start with a thorough physical examination and may conduct additional advanced diagnostics to gain a precise understanding of your knee's condition. This ensures every component of your treatment plan is perfectly matched to your specific joint anatomy and health status.
The treatment itself is focused on precision and your complete comfort.
Preparation: We begin by carefully cleansing the knee area, then apply a local anesthetic to ensure the entire experience is comfortable and pain-free.
Ultrasound-Guided Injection: Using a high-resolution ultrasound, our physician visualizes the inside of your knee in real-time. This allows for the precise placement of the allogeneic stem cell injection directly into the target area, ensuring the cells are delivered exactly where they are needed for maximum effect.
Post-Procedure Care: The entire procedure is typically completed in under an hour. Afterward, you will have time to relax in our recovery suite before we provide you with detailed instructions for your aftercare.
Our patient experience extends far beyond the medical procedure. Our dedicated concierge team is available to assist with all your travel and accommodation needs, ensuring your visit is as seamless and stress-free as possible. You can hear directly from patients who have undergone this journey by reading our patient testimonials.
A Holistic Approach to Recovery
We firmly believe that to achieve the full benefit of your stem cell therapy, it is essential to optimize your body’s internal environment for healing. That is why your treatment is integrated with supportive therapies designed to enhance your body's response and reduce systemic inflammation.
A successful outcome is not just about a precise injection; it is about creating the ideal biological conditions for your body to respond. Integrating therapies like hyperbaric oxygen and personalized IV infusions is how we elevate a standard procedure into a truly comprehensive regenerative program.
This integrated approach may include:
Hyperbaric Oxygen Therapy (HBOT): Breathing pure oxygen in a pressurized chamber enriches your blood with oxygen, which can help accelerate tissue repair and reduce swelling.
Personalized IV Infusions: We create custom nutrient infusions with powerful anti-inflammatory agents and key vitamins to support your cellular health and your body’s natural healing capacity.
This blend of advanced medical treatment and supportive wellness therapies defines our holistic commitment to your recovery. From the first call to your final follow-up, our team is dedicated to an experience that reflects the highest standards of both clinical excellence and patient care.
Your Questions About Stem Cell Knee Therapy Answered
Exploring regenerative medicine for your knees is an important step, and it is natural to have questions. This section is designed to provide clear, straightforward answers to the inquiries our patients most frequently have, so you can feel confident and informed about the path ahead.
Our commitment is to complete transparency, ensuring you feel secure and knowledgeable at every point in your health journey.
How Long Do the Benefits of Stem Cell Knee Injections Last?
This is one of the most common questions from patients, and the answer depends on your specific condition, age, and lifestyle. Many of our patients experience significant pain relief and improved knee function for anywhere from one to five years, and sometimes longer.
The goal is not a temporary fix; it is to modulate the inflammatory environment in your knee and support the health of your native tissues, which can successfully delay the need for surgery for years. We will create a personalized follow-up plan to track your progress and determine if any future maintenance therapy is appropriate to keep you feeling your best.
Is the Stem Cell Injection Procedure Painful?
We have designed the entire procedure to be as comfortable and minimally invasive as possible, a fact that often pleasantly surprises our patients. We use a local anesthetic to completely numb the area around your knee, which ensures you feel very little during the injection itself.
Our physicians perform the injection with absolute precision, using high-resolution ultrasound to guide the needle to the exact target within your joint. You may experience some mild, temporary soreness at the injection site for a day or two afterward, but this is a normal response and is easily managed with rest.
What Is the Recovery Process Like After the Procedure?
The recovery is dramatically different from that which follows a major surgery like knee replacement. It is significantly faster and far less demanding. Most patients return to light, day-to-day activities within a day or two.
We will ask you to avoid strenuous, high-impact activities for a few weeks. This is a crucial step—it gives the therapy the optimal environment to work effectively and allows your knee the time it needs to heal properly. You will leave with a personalized post-treatment plan to guide your recovery, help you strengthen the joint, and secure a positive long-term outcome.
We exclusively use allogeneic mesenchymal stem cells from carefully screened, healthy donors. This approach offers significant clinical advantages. Allogeneic cells are young, robust, and available in the high, standardized concentrations that are crucial for therapeutic efficacy.
This method also eliminates the need for an invasive harvesting procedure, simplifying the process and removing any potential discomfort from a donor site. Our on-site, COFEPRIS-licensed lab ensures these cells meet the highest international standards for safety, purity, and potency.
Our Commitment to Clinical Accuracy
Navigating the choice between stem cell therapy and knee replacement requires clear, trustworthy information. Our goal with this guide is to provide an honest, evidence-based perspective to help you make a confident decision about your health. To receive a personalized assessment of your condition, we invite you to schedule a consultation.
Author
Dr. Kirk Sanford, DC — Founder & CEO, Longevity Medical Institute. Dr. Sanford focuses on patient education in regenerative and longevity medicine, translating complex therapies into clear, practical guidance for patients.
Medical Review
Dr. Félix Porras, MD — Medical Director, Longevity Medical Institute. Dr. Porras provides clinical oversight and medical review to help ensure accuracy, safety context, and alignment with current standards of care.
Last Reviewed: Novemeber 18, 2025
Short Disclaimer
This information is for educational purposes only and is not medical advice. It does not replace an evaluation by a qualified healthcare professional. For personalized guidance, please schedule a consultation.