Exosomes vs Stem Cells: Choosing the Right Regenerative Therapy
When exploring advanced healing, the terms stem cells and exosomes often arise. Both are at the pinnacle of regenerative medicine, yet they serve fundamentally different roles in your body's repair processes. Understanding this distinction is the first, most crucial step in discovering which therapy is best aligned with your personal health goals.
At its core, the difference is this: stem cells are the builders that can create new tissue, while exosomes are the messengers that orchestrate cellular repair. Imagine the difference between needing new construction workers on-site versus requiring a clear set of blueprints for the skilled crew you already have. This central concept guides the choice between exosomes vs stem cells.
Understanding Regenerative Medicine's Leading Therapies
Regenerative medicine marks a profound shift away from merely managing symptoms. We are now able to work with the body's innate intelligence, empowering it to repair damage at a cellular level. Stem cells and exosomes are the two powerhouses leading this charge, but they function in very distinct ways.
Stem cells are the body's 'master cells,' possessing the remarkable ability to develop into specialized cell types—like cartilage, muscle, or bone. They are the skilled construction workers on your body's job site, capable of rebuilding damaged structures from the ground up. This makes them an exceptional choice for conditions where tissue has been significantly lost or worn down over time.
Exosomes, on the other hand, are not cells at all. They are microscopic 'messenger particles' released by cells, particularly stem cells. They cannot replicate or transform. Instead, they act as the project foremen, delivering a payload of vital instructions—proteins, growth factors, and genetic information—that direct your own cells to:
Reduce inflammation and pain signals.
Protect existing cells from further damage.
Stimulate the body's own natural repair mechanisms.
Accelerate recovery and healing.
Key Differences At A Glance
This quick comparison helps clarify the distinct clinical roles of exosomes versus stem cells.
The simplest way to frame the stem cells vs. exosomes debate is to ask: Does my body need new building blocks, or does it need better instructions for the blocks it already has? Answering this question is the first step toward a truly personalized treatment strategy.
This guide provides a clear, in-depth comparison to help you understand how these therapies work, their unique advantages, and which approach is best suited to help you achieve your specific health goals. For a solid grounding in this field, you can learn more about how regenerative medicine works in our detailed guide. This knowledge will put you in a position to make a confident, informed decision on your path to recovery.
To truly appreciate the difference between exosomes and stem cells, we must look deeper than their shared regenerative origins and examine how each functions at a biological level.
While both offer tremendous healing potential, their methods are fundamentally distinct. The most effective way to conceptualize this is through an analogy: stem cells are the skilled builders on a construction site, while exosomes are the meticulous foremen directing the entire project. This distinction is at the heart of choosing the right therapy for your specific needs.
Stem Cells: The Cellular Builders
Stem cells are living, complete cells that possess a unique ability to differentiate, meaning they can transform into other specialized types of cells. When we introduce mesenchymal stem cells (MSCs) into a damaged area, like an arthritic knee or a torn rotator cuff, they can become new cartilage, bone, or muscle cells.
This process involves a few key actions:
Engraftment: The stem cells physically embed themselves into the target tissue.
Differentiation: Taking cues from the local environment, they begin transforming into the specific cells needed for repair.
Proliferation: They then multiply, creating more cells to help rebuild the damaged structure over time.
Because they directly contribute to forming new tissue, stem cells are the gold standard for conditions where there's been significant structural loss or degeneration. They are the ‘boots on the ground’ solution for rebuilding what has been lost.
Exosomes: The Master Coordinators
Exosomes, on the other hand, are not cells. They are microscopic, acellular vesicles—tiny bubbles released by stem cells—packed with a sophisticated cargo of signaling molecules. This payload includes proteins, growth factors, and genetic material like mRNA and microRNA. They essentially act as the body’s internal communication network, delivering precise instructions to your existing cells.
Instead of becoming new tissue, exosomes work by modulating the behavior of your own cells. Their primary role is communication, not construction.
An exosome’s power lies not in its ability to become a new cell, but in its capacity to tell a population of your own cells how to behave more efficiently. They fine-tune the body’s innate healing response, reducing inflammation and activating regeneration without becoming part of the final structure.
This signaling function makes them incredibly versatile. You can learn more about how we apply these signaling capabilities in our detailed overview of exosome therapy. They are particularly effective for managing systemic inflammation, accelerating recovery, and promoting cellular health on a broad scale.
Comparing Functional Mechanisms
The different ways stem cells and exosomes work are clearly reflected in their clinical research and application. Stem cells have a much longer history of study, a fact highlighted by the sheer volume of clinical trials. There are currently over 7,018 clinical trials registered for stem cell therapies, compared to just 158 for exosomes.
This history has established stem cells as a proven therapy, with over 22,827 hematopoietic stem cell transplants performed annually in the U.S. alone for various conditions. Their power for direct repair is clear; a 2023 review noted that stem cells led to faster recovery in 75% of cases versus 50% for exosomes, underscoring their potency for structural rebuilding. You can read more about these comparative findings on exosomes and stem cells to see the data firsthand.
This table provides a clear breakdown of their functional differences, helping patients understand their key attributes at a glance.
Exosomes vs Stem Cells: A Detailed Feature Comparison
Ultimately, this 'builder' versus 'foreman' dynamic dictates which therapy is right for you. If your body needs new raw materials to rebuild a collapsing structure, stem cells are the logical choice. If it needs a master coordinator to manage the existing crew and accelerate the project, exosomes are often the superior tool.
When to Choose Exosomes or Stem Cells for Your Condition
Deciding between exosomes and stem cells isn't about selecting a universally "better" therapy. The right choice is entirely dependent on your specific condition, your body’s unique needs, and your ultimate health goals. A successful outcome hinges on matching the right tool to the right problem—whether that means physically rebuilding tissue or coordinating a complex healing response.
This section breaks down practical, real-world scenarios to guide your decision. We’ll explore how the fundamental differences between exosomes and stem cells translate into distinct clinical applications, helping you understand which path aligns with your desired outcome.
When Stem Cells Are the Preferred Choice
Stem cells are the clear choice when the primary goal is structural repair and tissue regeneration. If your condition involves significant tissue loss, damage, or degeneration that requires physical rebuilding, stem cells are uniquely equipped for the job. Their ability to become new tissue makes them the 'on-site construction crew' for your body.
Consider these common scenarios where stem cells excel:
Significant Orthopedic Injuries: For a condition like a torn ACL, a severe rotator cuff tear, or advanced cartilage loss in the knee, stem cells are often the superior choice. They can differentiate into new cartilage, ligament, and tendon cells, directly rebuilding the damaged joint structure to restore function.
Degenerative Disc Disease: When spinal discs have become significantly worn down and are causing chronic back pain, stem cells can be injected to help regenerate disc tissue, potentially restoring height and cushioning.
Osteoarthritis with Major Cartilage Loss: In the later stages of osteoarthritis where cartilage is substantially eroded, stem cells offer the potential to grow new cartilage. This addresses the root structural problem rather than just managing symptoms.
Think of it this way: If a wall has missing bricks, you need new bricks to fill the gaps. Stem cells are those new bricks, providing the raw materials necessary to reconstruct what has been physically lost.
This flowchart simplifies the core decision-making process, helping you visualize when to lean toward one therapy over the other based on your main objective.
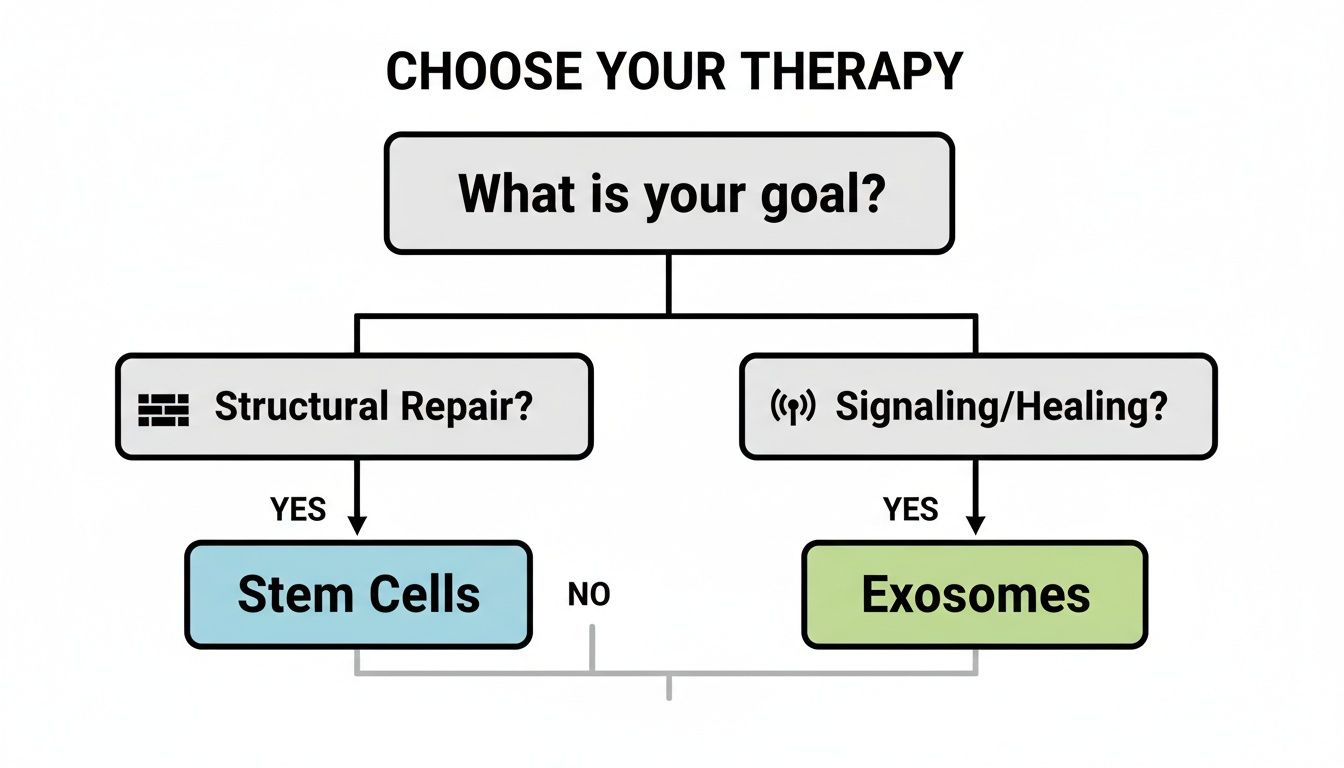
This decision tree shows that for fundamental structural repair, stem cells are the indicated path, while for managing the cellular environment through signaling, exosomes are the primary tool.
When Exosomes Are the Ideal Solution
Exosomes shine in situations where the main challenge isn't a lack of tissue, but rather a dysfunctional cellular environment characterized by widespread inflammation, poor signaling, and slow healing. As master coordinators, they excel at managing the body’s response to injury and stress.
Here are scenarios where exosome therapy is often the more targeted and effective approach:
Systemic Inflammation and Pain: For conditions driven by chronic, body-wide inflammation, such as early-stage osteoarthritis or some autoimmune-related joint pain, exosomes provide potent anti-inflammatory effects. They quiet down the "noise" of inflammatory signals, providing relief and creating a better environment for healing.
Accelerating Post-Surgical Healing: After orthopedic surgery, exosomes can be administered to manage inflammation, reduce scarring, and speed up recovery. They instruct local cells to repair tissue more efficiently, without the need for introducing new cells.
Aesthetics and Hair Restoration: For skin rejuvenation and stimulating dormant hair follicles, exosomes offer distinct advantages. Their small size allows for targeted delivery to stimulate collagen production and reawaken hair follicles, all without the complexities of cell-based therapy.
Research continues to highlight these nuanced roles. While stem cells often demonstrate more comprehensive regeneration in tissue repair, exosomes show remarkable versatility. For instance, studies have shown that certain exosomes can stimulate collagen production more effectively, showcasing their power in targeted aesthetic applications. The choice in the exosomes vs. stem cells debate truly comes down to the specific task at hand—building or directing.
Comparing the Safety and Risks of Each Therapy
When making a decision about your health, understanding the safety of a potential treatment is paramount. In the exosomes versus stem cells discussion, a transparent look at the risks and benefits is essential. Both are powerful tools in regenerative medicine, but their safety profiles differ because their fundamental biology is different.
At the Longevity Medical Institute, patient safety is the absolute foundation of our practice. We ensure every treatment, whether it involves stem cells or exosomes, adheres to the most stringent international standards for quality and purity.
The Safety Advantages of Acellular Therapy: Exosomes
Exosomes are widely considered to have an exceptional safety profile, and the reason is simple: they are acellular. This means they are not living cells. They are tiny vesicles carrying healing instructions, but they have no nucleus or DNA that can replicate. This one fact eliminates the most significant risks tied to cell-based therapies.
Key safety advantages of exosomes include:
Zero Risk of Replication: Because they are not alive, exosomes have no risk of multiplying, forming tumors, or causing uncontrolled growth. This is a critical distinction from any therapy involving living cells.
Minimal Immune Response: As non-living particles, exosomes are far less likely to be seen as "foreign" by your immune system. This makes rejection or an immune reaction extremely rare, ensuring they are highly compatible for almost every patient.
Exceptional Purity and Sterility: Exosomes are incredibly small, typically 30-150 nanometers. This allows them to be passed through nano-filters that screen out bacteria, viruses, and other contaminants, resulting in a pure, sterile, and safe final product.
The core safety advantage of exosome therapy lies in its acellular nature. By delivering only the healing messages without the cell itself, it sidesteps the most significant risks associated with cellular treatments, such as replication and immune rejection.
Evaluating the Risks of Stem Cell Therapy
Stem cell therapy has a much longer clinical history with decades of successful use. However, because the therapy involves administering living cells, there are inherent risks that must be managed with expert care. While these risks are low—especially when sourced and administered by specialists—it's important for patients to understand them.
Potential risks of stem cell therapy include:
Immune Reactions: When using donor cells (allogeneic therapy), there is a small potential for the patient’s immune system to recognize the cells as foreign and mount a response.
Uncontrolled Growth: While extremely rare with the mesenchymal stem cells (MSCs) used in regenerative medicine, there is a theoretical risk of unintended cell growth that must be monitored.
Infection Risk: As with any injection-based procedure, a risk of infection exists if rigorous sterility protocols are not followed meticulously.
Recent analyses highlight these safety differences, noting that safety profiles dramatically favor exosomes in many regenerative applications. While stem cells have been studied in over 7,018 clinical trials, they still carry moderate risks of immune rejection and other complications. In contrast, exosomes are emerging as a safer alternative in many contexts, with their low infection risk and lack of donor variability in standardized preparations.
At Longevity Medical Institute, we mitigate these risks through uncompromising quality control. Our on-site, COFEPRIS-licensed, and ISO-certified laboratory rigorously screens all biologics for purity, viability, and safety. For a deeper dive into our protocols for cell-based treatments, you can learn more about how we ensure stem cell therapy is safe for our patients. This meticulous process ensures that whether you choose stem cells or exosomes, you are receiving the highest standard of care available.
The Future of Healing: Combining Exosomes and Stem Cells
The conversation in advanced medicine is no longer about “exosomes vs. stem cells.” That is an outdated debate. The most forward-thinking clinical approach recognizes that the greatest results often come from using them together.
At the Longevity Medical Institute, we’ve moved beyond this binary choice. We now pioneer personalized protocols that combine both therapies for powerful, synergistic effects.
This integrated strategy allows us to address complex conditions from multiple angles, using each biologic for its unique strengths. It’s about creating a comprehensive healing environment where structural repair and cellular communication work in perfect concert.
Crafting Synergistic Patient Protocols
Our approach is tailored to the individual, creating a treatment plan that addresses the root cause of dysfunction with absolute precision. By combining therapies, we can orchestrate a more robust and efficient healing cascade than either could ever achieve alone.
Take a patient with severe, degenerative knee osteoarthritis. The primary issue is the physical loss of cartilage, which requires structural rebuilding. In this case, a targeted injection of mesenchymal stem cells (MSCs) directly into the joint provides the essential ‘builders’ to begin regenerating new cartilage tissue.
But the joint is also a highly inflammatory environment, which can hinder the new cells' ability to survive and thrive. This is where exosomes become critical. Following the stem cell injection, we administer exosome therapy to:
Drastically reduce local inflammation, creating a healthier, more receptive environment for the new stem cells.
Signal existing cells to support the healing process and protect against further degradation.
Promote the integration of the new stem cells, ensuring they can effectively engraft and begin their reparative work.
By pairing the “builders” (stem cells) with the expert “foremen” (exosomes), we create an optimized system for regeneration. The stem cells provide the structure, while the exosomes manage the site, ensuring the project runs smoothly and efficiently.
Applications Beyond Orthopedics
This combined approach extends far beyond just joint repair. A patient focused on comprehensive anti-aging and enhanced cognitive function may benefit from a different kind of synergy.
Their protocol might involve systemic IV exosome therapy to lower body-wide inflammation and improve cellular communication throughout the brain and body.
This foundational treatment could then be amplified with specialized peptides to target specific pathways, like cognitive function or metabolic health, and sessions of hyperbaric oxygen therapy (HBOT) to further boost cellular energy and regeneration. To learn more about how these therapies are used in combination, we have a detailed resource on our integrated stem cell and exosome treatments.
Our ability to design these advanced protocols is powered by our in-house, COFEPRIS-licensed biotechnology lab. This unique capability allows our physicians and scientists to create customized, high-potency treatments on-site. It ensures unparalleled quality control and delivers outcomes that a single-therapy approach simply cannot match. This is the future of personalized regenerative medicine.
How to Start Your Regenerative Medicine Journey
We’ve explored the powerful, distinct roles of exosomes and stem cells. You now understand that stem cells can act as the 'builders' for direct structural repair, while exosomes are the expert 'foremen' carrying the critical instructions for cellular communication.
But the most important takeaway is this: the best therapy is never a one-size-fits-all solution. It’s the one precisely matched to your unique biology, your specific condition, and your personal health objectives.
Your journey toward optimal health begins not with choosing a therapy, but with an expert evaluation to determine which therapy will choose you. A thorough diagnostic process is the foundation of any successful regenerative protocol.
We invite you to schedule a consultation with our dedicated medical team to discuss your goals in detail. Through advanced diagnostics and a comprehensive personal assessment, we will design a personalized treatment plan that empowers you to take control of your health and longevity.
Understanding your options for wellness with stem cell and exosome therapy in Mexico is the first step toward reclaiming your vitality. Our team is here to guide you with clarity and expertise.
Your Questions, Answered
Making an informed decision about your health requires clear, direct answers. It’s natural to have questions when exploring advanced therapies, so we’ve addressed the most common inquiries our patients have about exosomes and stem cells.
Our goal is to give you the clarity and confidence you need to choose the best path forward for your health.
How Long Do the Effects of These Therapies Last?
This is an excellent question, and the answer truly depends on the therapeutic goal. Stem cell therapy is aimed at creating long-term, and in some cases permanent, structural change. By helping the body regenerate new tissue, it can offer a lasting solution for degenerative conditions.
Exosome therapy, on the other hand, delivers powerful signaling benefits that quiet inflammation and kickstart the body’s own repair processes. These effects can last for many months, but for chronic conditions, periodic treatments might be recommended to maintain that anti-inflammatory edge and keep your cells functioning optimally.
Can Exosomes and Stem Cells Be Used Together?
Absolutely. In fact, this is often our preferred method at Longevity Medical Institute. We frequently design synergistic protocols to achieve the most comprehensive results.
For example, we might inject stem cells directly into a damaged knee joint to help rebuild cartilage, while also administering exosomes systemically to manage the inflammatory response. This helps accelerate the overall healing process and supports the new cells as they get to work.
This combined strategy leverages the "builder" role of stem cells and the "foreman" role of exosomes at the same time, creating a more powerful, well-orchestrated outcome.
What Is the Recovery Time for These Treatments?
The recovery for each therapy is quite different. Exosome therapy is a cell-free treatment that is minimally invasive, so it typically involves little to no downtime. Most patients are able to return to their normal activities immediately.
Stem cell injections, particularly for orthopedic conditions, may require more planning. We often recommend a short period of rest followed by a structured rehabilitation plan. This is crucial for protecting the newly forming tissue and ensuring you get the best possible results from the therapy.
Are These Treatments Safe for International Patients?
Yes, patient safety is the absolute foundation of our practice at Longevity Medical Institute. We operate a fully COFEPRIS-licensed medical facility and adhere to the highest international safety and quality standards.
Our in-house, state-of-the-art lab ensures every biologic we use is rigorously tested and prepared on-site. This provides an unparalleled level of safety and quality assurance for all our patients, especially those traveling from abroad for their care.
Your journey toward optimal health begins with an expert evaluation. We invite you to schedule a consultation with our medical team at Longevity Medical Institute to discuss your goals. Through advanced diagnostics and a thorough assessment, we will design a personalized treatment plan that empowers you to take control of your health and longevity. Schedule your consultation today.
Author
Dr. Kirk Sanford, DC — Founder & CEO, Longevity Medical Institute. Dr. Sanford focuses on patient education in regenerative and longevity medicine, translating complex therapies into clear, practical guidance for patients.
Medical Review
Dr. Félix Porras, MD — Medical Director, Longevity Medical Institute. Dr. Porras provides clinical oversight and medical review to help ensure accuracy, safety context, and alignment with current standards of care.
Last Reviewed: March 5, 2026
Short Disclaimer
This information is for educational purposes only and is not medical advice. It does not replace an evaluation by a qualified healthcare professional. For personalized guidance, please schedule a consultation.