Stem Cells for Inflammation Reduction: A Patient's Guide
Some people arrive at this question after months or years of feeling “off.” Their joints ache without a clear injury. Their recovery is slower than it used to be. Energy dips. Sleep becomes lighter. Brain fog comes and goes. Standard tests may explain part of the story, but not all of it.
A common thread in many of these cases is chronic inflammation, often driven by a process known as inflammaging, a persistent, low-grade inflammatory state that develops with age and contributes to the progression of many chronic diseases.
When inflammation stops being a short-term healing response and becomes a steady background signal, it can affect how you feel almost everywhere in the body. That’s why interest in stem cells for inflammation reduction has grown so quickly. Patients aren’t only asking whether regenerative medicine can help a sore knee. They’re asking whether it can help calm the larger inflammatory pattern behind pain, fatigue, stiffness, and slower healing.
At a clinical level, that’s the right question.
The Hidden Driver of Disease: Understanding Chronic Inflammation
Inflammation isn’t automatically harmful. In the right setting, it’s protective. If you cut your hand or catch a virus, your immune system sends signals that help defend and repair.
The problem starts when that alarm never fully switches off.
A useful analogy is a car engine running hotter than it should. It may still move, but the extra heat gradually wears down hoses, seals, and moving parts. Chronic inflammation, or inflamaging, behaves in a similar way. It creates low-grade biological stress that can irritate tissues, disrupt normal repair, and accelerate wear across multiple systems.
Why it feels so hard to define
Many patients expect inflammation to look obvious, like redness, swelling, or a fever. Chronic inflammation often doesn’t behave that way. It can be quieter and more diffuse.
You may notice patterns such as:
Persistent soreness: Joints, muscles, or tendons feel irritated more often than they should.
Slow recovery: Exercise, travel, poor sleep, or stress affect you more than they once did.
Brain and mood changes: Concentration feels less sharp, and resilience feels lower.
Whole-body fatigue: You rest, but you don’t feel restored.
These symptoms can overlap with many conditions, which is why people often feel confused. They know something is wrong, but the problem doesn’t fit neatly into a single category.
Inflammaging and the bigger picture
In longevity medicine, we often use the term inflammaging. It describes the way chronic, systemic inflammation contributes to biological aging over time. Inflammation isn’t solely associated with pain; it also influences tissue quality, immune balance, vascular health, and cognitive function.
Chronic inflammation is less like a single disease and more like an unfavorable operating environment for the body.
That’s why symptom suppression alone often feels incomplete. A patient may temporarily feel better with anti-inflammatory medications, but if the underlying immune signaling remains dysregulated, the body can keep returning to the same inflammatory pattern.
Why patients start looking beyond symptom control
This is usually the turning point. People begin asking a different kind of question. Not “What can numb this symptom?” but “What can help reset the environment that keeps producing it?”
That’s where regenerative medicine becomes relevant. The goal isn’t to block inflammation for a few hours or days. The goal is to help the body shift from an overactive inflammatory state toward a more balanced repair state.
For the right candidate, that’s a much more meaningful therapeutic direction.
How Stem Cells Calm Inflammation: The Science of Cellular Healing
A patient arrives at an international regenerative medicine clinic after years of chasing the same pattern. Joint pain flares, brain fog intensifies, gut symptoms settle briefly, then return. Standard anti-inflammatory drugs may quiet the noise for a time, yet the immune system keeps behaving like an alarm that was never properly reset.
That is the clinical problem cell therapy is designed to address.
Most patients first view stem cells as replacement material. In inflammation care, mesenchymal stem cells, or MSCs, are better understood as cellular coordinators. Their main value often comes from what they signal, not from becoming large amounts of new tissue.
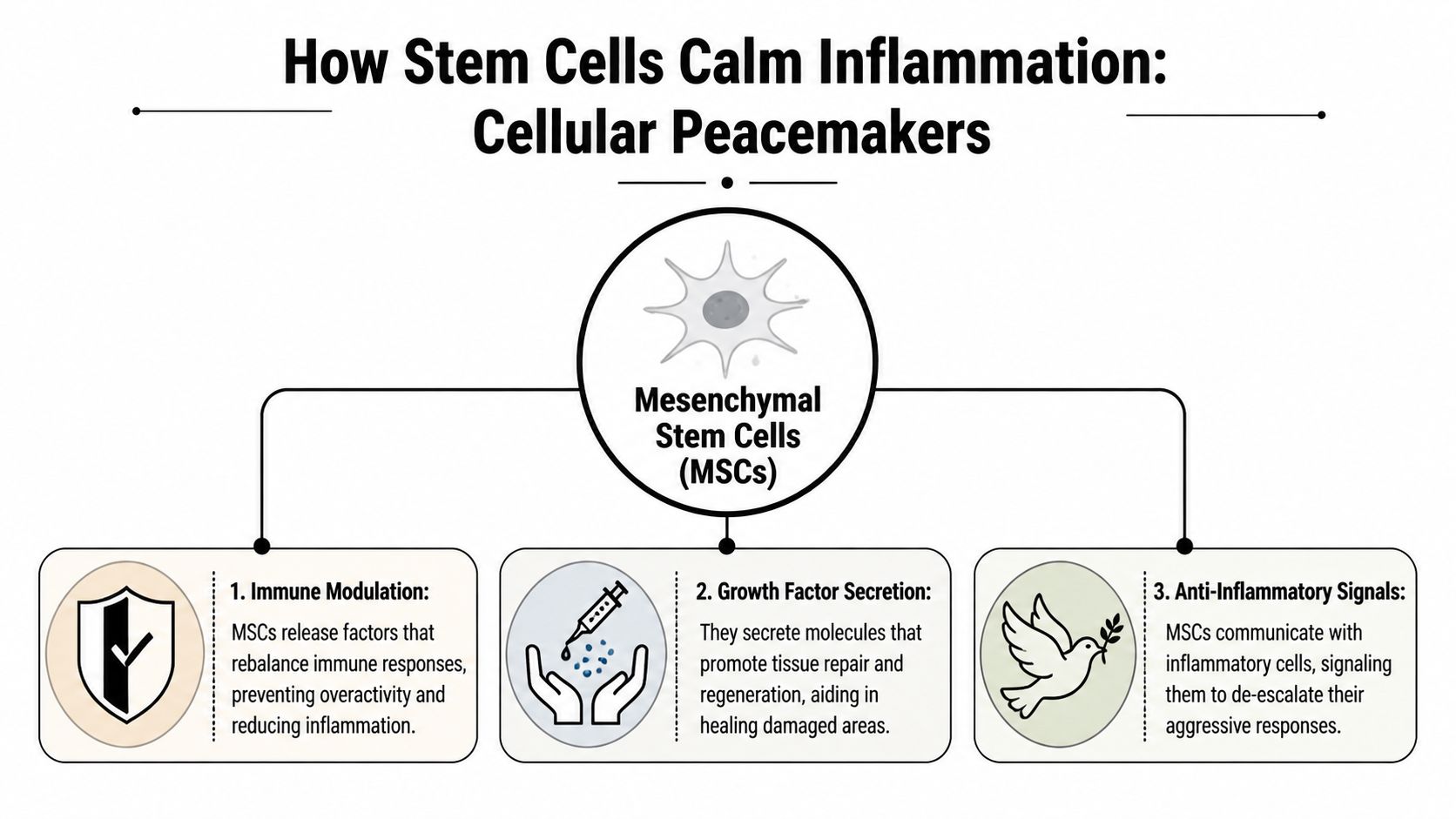
They act more like conductors than bricks
An orchestra works only when each section responds to the same score. MSCs serve a similar role inside an inflamed body. They enter a biologically noisy environment, detect the surrounding inflammatory signals, and release molecules that influence how immune and repair cells behave.
If you’d like a broader foundation before going deeper into mechanism, this explanation of how stem cell therapy works pairs well with the science below.
Clinicians call this paracrine activity. In plain language, MSCs send out a biochemical message package that includes cytokines, growth factors, lipid mediators, and extracellular vesicles. Those messages can change the behavior of nearby cells and, in some cases, reshape wider immune signaling throughout the body.
The macrophage shift patients should understand
One of the clearest examples involves macrophages. These immune cells help determine whether the body remains in a defensive inflammatory state or transitions into repair.
A simplified framework looks like this:
| Macrophage state | Functional tendency |
|---|---|
| M1 | More pro-inflammatory, defensive, and aggressive |
| M2 | More anti-inflammatory, restorative, and pro-regenerative |
MSCs can help shift macrophages from an M1 profile toward an M2 profile. According to a peer-reviewed review on MSC immunomodulation, MSCs use paracrine-mediated reprogramming to convert pro-inflammatory macrophages from Type 1 (M1) to Type 2 (M2). The same review describes increased secretion of anti-inflammatory cytokines, particularly interleukin-10 (IL-10), along with reduced expression of pro-inflammatory cytokines such as IL-1β and IL-17. It also identifies TSG-6 as a validated surrogate biomarker of therapeutic activity. You can also review this study Mesenchymal Stromal Cells as Modulators of Chronic Inflammation, Inflammaging, and Age-Related Disease: A Systematic Review.
For patients, the translation is straightforward. The therapy aims to interrupt escalation and support a repair-oriented immune response.
Clinical insight: The goal is rarely blunt immune shutdown. The goal is a more orderly immune response.
Why short-lived cells can still create lasting effects
This point often causes confusion. Patients understandably assume a cell must remain in the body for months or years to matter. In many inflammation protocols, that is not the primary mechanism.
MSC therapy may act more like pressing a reset sequence than installing a permanent part. The cells can interact with monocytes, macrophages, and other immune cells early after administration, then leave behind changes in signaling behavior that persist beyond the cells themselves. For clinicians, that changes how success is measured. We focus not only on cell persistence, but on whether the inflammatory network has been redirected toward resolution.
That distinction matters in real-world protocol design at high-level international clinics. An advanced allogeneic program does not merely ask, “How many cells were given?” It asks sharper questions. Which inflammatory pattern is dominant? Which route of administration best matches that pattern? Is the objective systemic immune recalibration, tissue-level repair support, or both?
They respond to the environment they enter
MSCs are not passive. They are highly responsive to context.
A body with active inflammatory signaling presents one molecular environment. A body with lower inflammatory burden presents another. MSCs respond differently depending on those cues, which is one reason treatment quality depends heavily on sourcing, processing, timing, dose selection, and route of delivery.
For medical travelers, this is an important distinction between generic marketing and genuine protocol-based care. At a premier clinic, the treatment plan is built around the patient’s inflammatory profile, medical history, laboratory findings, and travel timeline. The science is elegant, but the practical goal is simple. Help the immune system stop overreacting and start coordinating repair more intelligently.
Advanced Allogeneic Therapies: The Power of Young Potent Cells
When patients hear the term allogeneic, they often pause. It means the cells come from a carefully screened donor source rather than from the patient’s own body.
In inflammation-focused regenerative care, that distinction matters.
Why clinics use allogeneic cells for systemic inflammation
A patient seeking help for chronic inflammation is often dealing with a body-wide problem, not just a local injury. In that setting, clinicians want cells with strong signaling capacity, consistent quality, and predictable behavior.
A review on MSC biology explains that these cells demonstrate context-responsive immunomodulation, and their low immunogenicity allows allogeneic, off-the-shelf deployment without concurrent immunosuppression. It also notes that this property has been validated by regulatory approval in Canada and New Zealand for treating graft-versus-host disease, and that reproducible outcomes depend on precise protocol design, standardization, and evidence-based clinical use, as summarized in this review of MSC immunology and therapeutic translation.
That matters for two reasons:
Consistency: The product can be prepared under controlled laboratory conditions rather than varying from patient to patient.
Readiness: Therapy can be delivered without the extra procedural step of collecting cells from the patient first.
The five cell types used in our lab
For educational clarity, it helps to know that not all cell preparations are identical. Our biotechnology lab produces five different types of stem cells:
Placental cells: Often selected when clinicians want broad regenerative signaling support.
Wharton’s jelly cells: Commonly discussed in anti-inflammatory and musculoskeletal applications because of their strong paracrine activity.
Adipose-derived cells: Relevant in regenerative protocols where connective tissue support is part of the treatment strategy.
Endometrial cells: Studied for their regenerative signaling and repair-oriented behavior.
Dental pulp cells: Of interest for neuro-supportive and repair-focused applications.
A separate overview of umbilical stem cell therapy can help if you want to compare tissue sources in more detail.
What patients often misunderstand about safety
Many people assume donor-derived cells must automatically create rejection. That assumption comes from organ transplantation, where long-term tissue matching is critical. MSC therapy is different. These cells are valued in part because of their low immunogenicity and their ability to modulate immune activity rather than provoke it.
That doesn’t mean every product is equal. It means sourcing, cell characterization, handling, and protocol design matter enormously.
The conversation shouldn’t be “allogeneic or not.” It should be “how were these cells sourced, processed, and used?”
Where exosomes fit
Some patients also ask about exosomes. A practical way to think of them is this: if stem cells are the communication hub, exosomes are part of the message delivery system. They carry signaling cargo that can support anti-inflammatory and reparative communication without administering whole cells.
In clinical practice, physicians may consider cell therapy, exosome therapy, or a combination approach depending on the patient’s goals, inflammatory burden, anatomy, and timeline.
Clinical Applications and Published Evidence
The strongest way to understand stem cells for inflammation reduction is to look at where inflammation drives disease most clearly. In practice, three broad categories come up most often: orthopedic degeneration, autoimmune or immune-mediated illness, and systemic inflammatory states that affect energy, cognition, and resilience.
Orthopedic conditions
Joint disease is one of the clearest entry points because inflammation and tissue degeneration often reinforce each other. A painful knee, shoulder, hip, or spine segment may not merely be “worn out.” It may also be living in a persistently inflamed microenvironment that interferes with repair.
Published data summarized in this article of stem cell therapy success rates across conditions reports that 60 to 80 percent of patients with orthopedic issues delay or avoid joint replacement after stem cell therapy. The same source notes that 60 to 80 percent of patients with osteoarthritis and joint degeneration experience meaningful improvement.
For patients, these numbers are best interpreted as evidence of meaningful clinical potential, not as a guarantee. The right question isn’t whether every person will respond the same way. It’s whether the biology of your condition makes you a reasonable candidate for a regenerative anti-inflammatory strategy.
Autoimmune and immune-mediated disorders
This category is more complex because the immune system itself is misdirected. The therapeutic goal is not limited to soothing a local area. It’s to help rebalance immune signaling that has become chronically disruptive.
The same published summary reports that for multiple sclerosis, patients receiving autologous hematopoietic stem cell transplants showed 19 percent improvement in disability over five years, compared with 4 percent in medication-only controls. While that specific data point involves a different transplant category than allogeneic MSC therapy, it still supports a larger principle. Cell-based therapies can meaningfully change inflammatory disease trajectories in the right setting. You can learn more in this guide, Unlocking Hope: Stem Cells in Multiple Sclerosis Treatment.
Patients often ask whether this means stem cell therapy “cures” autoimmune disease. That’s not the right frame. A more accurate clinical frame is immune modulation, symptom reduction, support for function, and, in some cases, a shift toward greater stability.
Systemic inflammatory conditions
Some inflammatory illnesses don’t stay confined to a single tissue. Patients with chronic inflammatory burden may describe diffuse pain, cognitive slowing, post-viral changes, exercise intolerance, or a sense that their body never fully resets.
Systemic administration is particularly clinically interesting, as the same evidence summary reports that in chronic heart failure, the largest cell therapy trial showed a 58 percent reduction in heart attack or stroke risk, which increased to 75 percent in patients with high inflammation. That finding is important because it suggests that anti-inflammatory cell therapy can have effects well beyond a single injection site.
A thoughtful discussion of published stem cell safety findings can help patients evaluate the broader body of evidence alongside efficacy.
What to take from the evidence
A simple way to organize the clinical picture is this:
Orthopedic disease: Often involves local inflammation plus structural decline.
Autoimmune illness: Often involves immune misdirection and ongoing tissue irritation.
Systemic inflammatory syndromes: Often involve widespread signaling imbalance rather than a single lesion.
The common denominator is immune dysregulation. That’s why MSC-based therapies attract so much clinical interest across apparently different diagnoses.
Your Treatment Journey: A Personalized Path to Wellness
For most patients, the treatment journey starts before any infusion or injection. It starts with pattern recognition. You know your symptoms may share an inflammatory root, but you also know that guessing isn’t good enough.
That’s why a serious regenerative workup should begin with evaluation, not sales language.
The first step is clarifying the pattern
A physician-led review usually focuses on a few core questions:
Where is the inflammation showing up most clearly? Joints, gut, skin, nerves, cognition, energy, or several at once.
What has already been tried? Medications, injections, rehabilitation, supplements, or other therapies.
Is this mostly local, systemic, or both? That distinction shapes route and protocol.
A more advanced program may add in-house biomarker testing and imaging to sharpen the picture. At some clinics, that includes a broad internal lab panel, advanced cardiac screening, and full-body MRI integrated with AI review so treatment decisions are guided by measurable findings rather than symptom labels alone.
What treatment day usually feels like
Patients are often relieved to learn that the day itself is usually straightforward. If the plan is systemic, treatment may involve an intravenous infusion. If the target is more focused, such as a joint or tendon, an image-guided injection may be used.
The experience is generally calm and structured. Vital signs are monitored. The clinical team reviews the plan. Patients usually spend treatment time resting rather than “recovering” in the surgical sense.
What matters most on treatment day: precise protocol, appropriate route, and careful patient selection.
Why supportive therapies may be added
A regenerative program often works best as a coordinated plan rather than a single isolated event. Depending on the patient, physicians may pair stem cell therapy with supportive options such as physical medicine, targeted rehabilitation, IV strategies, or hyperbaric oxygen.
The reason is simple. If the goal is to calm inflammation and improve tissue function, you want the surrounding environment to support that shift.
A patient with joint degeneration may need movement retraining. A patient with systemic inflammatory stress may need recovery support and metabolic stabilization. A patient with travel fatigue may need scheduling that protects rest and hydration.
For medical travelers, logistics matter too
Patients traveling from the United States or Canada usually care about more than the cells themselves. They want to know who coordinates the airport transfer, where they’ll recover, how follow-up works, and whom they can contact after returning home.
A well-run program addresses those questions early. The clinical process should feel organized, medically grounded, and easy to follow even when the science is advanced.
That’s especially important in regenerative medicine, where the patient experience can strongly influence comfort, adherence, and confidence in the care plan.
Benefits Risks and Practical Guidance for Medical Travel
A patient often reaches this stage with two competing thoughts. “This could help.” “I do not want to travel for something I do not fully understand.”
That hesitation is reasonable.
For medical travelers considering allogeneic cell therapy, the essential question is not only whether stem cells can reduce inflammation. It is whether the clinic uses disciplined protocols, screens patients carefully, and manages the trip with the same rigor as the treatment itself. In a serious program, those pieces belong together.
The benefit patients usually notice first is practical. Less pain. Easier movement. Better exercise tolerance. Clearer thinking in some cases where systemic inflammation has been part of the picture. The deeper goal sits below symptoms. Physicians are trying to interrupt an overactive inflammatory loop and shift the body toward a more regulated state.
That is why benefit can outlast the brief presence of the administered cells. As noted earlier, mesenchymal signaling often matters more than long-term cell residence. The cells act more like a short clinical conversation with the immune system than a permanent transplant. If the message is well matched to the patient, the downstream effect can continue after the cells themselves are no longer circulating.
A balanced view of risks
Good regenerative medicine starts with selection.
Some patients are appropriate candidates. Others are better served by delaying treatment, changing the plan, or avoiding cell therapy altogether. Active infection, poorly controlled disease, clotting concerns, recent instability, or goals that do not match the biology all need careful review. A responsible physician also asks a harder question many clinics skip. Is inflammation driving the problem, or is it only one small piece of it?
That distinction matters. A patient with inflammatory joint pain may have a clear therapeutic target. A patient with advanced structural damage and little remaining tissue function may still be helped, but the expected outcome is different. Inflammation can be quieted. Anatomy is not always rebuilt.
Patients who want a grounded overview before booking often begin with this guide to stem cell therapy safety in Mexico.
What to verify before you travel
International care adds another layer of decision-making. The science can be sound, yet the experience still goes poorly if logistics, documentation, or follow-up are weak.
Ask direct questions:
Where do the cells come from? Confirm allogeneic sourcing, donor screening, sterility standards, and release testing.
Who decides your protocol? A physician should determine candidacy, dosing logic, route of administration, and whether adjunctive therapies are appropriate.
What happens after treatment? You should know how the clinic handles follow-up, symptom updates, and communication once you are back home.
How is the trip organized? Airport transfer, lodging coordination, treatment-day timing, and recovery support should be clear before arrival.
What is the regulatory framework? Patients traveling abroad should understand how the clinic describes licensure, laboratory standards, and clinical oversight.
One sentence can save a great deal of confusion. Ask the clinic to explain your treatment plan in plain language, as if they were briefing a family member.
Good regenerative care feels clear before you arrive and structured after you leave.
One factual example in this space is Longevity Medical Institute in San José del Cabo, which describes a physician-led model with in-house clinical laboratory capabilities, advanced imaging, and access to a COFEPRIS-licensed, ISO-certified biotechnology lab. For a medical traveler, that operational detail matters because it tells you how decisions are made, how quality is documented, and who is accountable if questions come up during the process.
In other words, the trip should feel medically organized, not arranged around marketing. That is often the difference between a clinic that offers stem cells and a clinic that runs a true allogeneic cell therapy program.
Frequently Asked Questions
How long does it take to see results from stem cell therapy
There isn’t one universal timeline. Some patients notice early changes in pain, stiffness, or energy, while others improve gradually as inflammation settles and tissue recovery progresses. The timeline depends on whether the problem is local or systemic, how long it has been present, and what else is affecting healing.
A useful mindset is to think in phases: early immune modulation, then functional improvement, then longer-term stabilization if the treatment was well matched.
Is stem cell therapy a permanent cure
Usually, that’s not the right expectation. Stem cell therapy is better understood as a way to help regulate inflammation, support repair, and improve function. Whether that benefit lasts depends on the condition being treated, the patient’s biology, and what ongoing stressors remain.
If someone has severe inflammatory triggers from poor sleep, high stress, metabolic dysfunction, or repetitive joint overload, those factors still matter after treatment.
How do I know if I’m a good candidate
Good candidates usually share three features. First, inflammation appears to be a meaningful part of the problem. Second, there’s a realistic therapeutic target, such as symptom reduction, improved function, or recovery support. Third, the patient understands that regenerative medicine works best inside a broader care plan.
A formal review should include medical history, current diagnoses, medications, prior treatments, and a discussion of risks and alternatives.
What makes allogeneic cells different
Allogeneic cells are donor-derived cells prepared for clinical use rather than harvested from the patient at the time of treatment. Their value lies in consistency, availability, and strong signaling potential when processed under appropriate standards.
That said, “allogeneic” alone doesn’t tell you enough. You still need to ask about source tissue, laboratory controls, viability, protocol design, and clinical oversight.
What about side effects
Every medical treatment deserves an honest discussion of side effects and risk. That includes regenerative medicine. If you want a practical patient overview, this article on stem cell therapy side effects is a useful place to start.
The most important point is that candidacy and protocol matter. The goal isn't limited to receiving cells. It's to receive the right treatment for the right reason in the right setting.
Begin Your Journey Toward Renewed Vitality
You may have reached this point after months, or years, of feeling slightly less like yourself. Energy is less reliable. Recovery takes longer. Pain, stiffness, or mental fog begin to shape daily decisions. For many patients, especially those traveling for care, the question is not whether inflammation matters. It is whether there is a clear, medically supervised plan to address it.
Stem cells for inflammation reduction represent that kind of plan when used thoughtfully. In a well-designed allogeneic protocol, the goal is not to chase every symptom one by one. The goal is to influence the immune signals that keep the body stuck in a cycle of irritation and incomplete repair. A useful comparison is resetting an orchestra after the instruments have drifted out of tune. The cells are not replacing the whole system. They are helping restore coordination.
At a physician-guided clinic, that process begins long before treatment day. The medical team reviews history, imaging, laboratory findings, current medications, prior interventions, and travel logistics. For international patients, practical details matter. Timing, follow-up, recovery expectations, and fit for travel all need to be clear before any protocol is approved.
Clarity changes the experience.
Once patients understand how allogeneic cell therapy is selected, prepared, and matched to a clinical objective, the treatment usually feels less abstract. It becomes a structured medical decision with defined goals, defined monitoring, and a realistic view of what improvement may look like over time.
That is the standard patients should expect. Clear reasoning. Careful screening. Treatment that fits the person, not just the diagnosis.
Author
Dr. Kirk Sanford, DC, Founder & CEO, Longevity Medical Institute. Dr. Sanford focuses on patient education in regenerative and longevity medicine, translating complex therapies into clear, practical guidance for patients.
Medical Review
Dr. Félix Porras, MD, Medical Director, Longevity Medical Institute. Dr. Porras provides clinical oversight and medical review to help ensure accuracy, safety context, and alignment with current standards of care.
Last Reviewed: May 5, 2026
Short Disclaimer
This information is for educational purposes only and is not medical advice. It does not replace an evaluation by a qualified healthcare professional. For personalized guidance, please schedule a consultation.